Sickle cell disease disproportionately affects populations in Africa and India, however advancements in gene therapy are not widely accessible.
Gautam Dongre has two children residing in India and Pascazia Mazeze has a son living in Tanzania who both suffer from an inherited blood disorder that causes their blood cells to cause excruciating pain.
Dongre expressed hope for a cure for their sickle cell disease through new gene therapies, stating that he is praying for the treatment to become available to them.
However, according to specialists, the single-dose remedy is not accessible in India and Africa, which are the regions with the highest prevalence of the disease. Widespread disparities prevent a significant portion of the global population from accessing gene therapy in general.
In developing nations, there is a limited availability of various types of medication. However, the issue is particularly severe with these treatments, as they are some of the most costly in the world.
In addition to their exorbitant costs, administering these treatments to patients is highly intricate and involves extended hospital stays, advanced medical technology, and specialized physicians and researchers. Currently, the two approved gene therapies for sickle cell are only available in more affluent nations – with both being approved in the U.S. and one each in Britain and Bahrain.
Dr. Benjamin Watkins, a physician who specializes in treating sickle cell disease in New Orleans and also works with children globally, expressed that the overwhelming majority of patients reside in regions without access to this particular form of treatment. He emphasized the need for the medical community and society as a whole to consider this issue.
The international summit on human genome editing in London placed significant emphasis on access to gene therapies. According to a recent editorial in the journal Nature, the steep cost of these therapies could greatly hinder progress in the field and leave low- and middle-income countries at a disadvantage.
Certain researchers have concerns that potential advancements in medicine may not be fully realized, leading to a lack of future treatments and preventing the eradication of diseases such as sickle cell from becoming a reality.
Having difficulty receiving essential medical care
In order for gene therapy to be a possibility, individuals living in developing countries must survive long enough to receive it. In these regions, sickle cell disease is more likely to cause severe disability or death compared to more affluent areas. A delayed diagnosis is frequent and access to basic medical care can be limited.
According to Watkins from Children’s Hospital New Orleans, although gene therapy is a significant advancement, we must not overlook the needs of our patients.
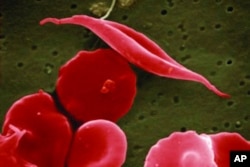
At birth, sickle cell disease starts to attack the body by impacting hemoglobin, the protein responsible for carrying oxygen in red blood cells. Due to a genetic mutation, the cells take on a crescent shape, potentially obstructing blood flow and leading to issues like severe pain, organ damage, and stroke.
Another potential treatment is a bone marrow transplant, but it requires a donor who is closely matched and carries the risk of rejection.
The estimated global population affected by this disease ranges from 6 million to 8 million, although exact numbers are uncertain. This disease is more prevalent in areas prone to malaria, as having the sickle cell trait can provide some protection against severe cases. Research suggests that over 1 million individuals with sickle cell disease reside in India, and over 5 million are located in sub-Saharan Africa.
Dongre, who lives in Nagpur in central India, has seen the struggles in his own family and among people he’s met as a leader in the National Alliance of Sickle Cell Organizations in India. For many years, awareness of the disease has been lacking, he said, even among some health professionals.
Dongre shared the story of his infant son, Girish, who suffered from persistent crying due to stomach and leg discomfort. Despite seeking medical help, doctors were unable to identify the issue and it took 2-1/2 years before he was diagnosed with sickle cell disease. When their second child, Sumedha, was born, they wasted no time in getting her tested and discovered she also had the disease.
Many individuals are not diagnosed with sickle cell disease until ten years or more have passed. Lalit Pargi, a resident of Udaipur in northern India, did not receive a diagnosis until he was 16 years old, even though he displayed the classic symptoms of jaundice, such as yellow eyes and skin, which are often associated with sickle cell disease. This resulted in a childhood filled with unexplained pain.
‘God and Google’
There are treatments available to lessen the episodes of pain referred to as “crises.” Dongre’s two children, who are currently 19 and 13 years old, are prescribed a medication called hydroxyurea. This medication, which has been used for decades as a chemotherapy drug, helps prevent the development of sickle-shaped red blood cells and manages the symptoms of the disease. Both children have been admitted to the hospital for pain episodes, particularly when they were younger.
According to Dongre, there are other individuals living in rural regions who are passing away at a young age due to lack of proper medical care.
In July, the Prime Minister of India, Narendra Modi, initiated a campaign to eliminate sickle cell disease. This initiative includes promoting awareness, providing education, conducting screenings, and encouraging early detection and treatment. Dongre expressed appreciation for the effort, but also acknowledged the significant challenges that the country must overcome in order to achieve its objectives.
The scenario is similar in Tanzania, located in East Africa, where the Ministry of Health has collaborated with Novartis, a pharmaceutical company that produces medication for sickle cell disease, in order to enhance access to diagnosis and treatment.
Mazeze frantically searched for information following her son’s diagnosis of Ian Harely.
Mazeze, the executive director of the Tanzania Sickle Cell Warriors Organization, searched repeatedly on Google and was unable to sleep. Following that, he turned to prayer, acknowledging the help of both God and Google.
Her son is now 10 and takes hydroxyurea and folic acid for anemia. They’ve helped but haven’t eliminated pain episodes like the one that put him in the hospital for two weeks earlier this year.
However, Mazeze considers herself fortunate that she is able to pay for medical treatment.
According to her, there are individuals in Tanzania who struggle to afford folic acid. The cost for a month’s supply of folic acid is 1,000 Tanzanian shillings, which is equivalent to less than one US dollar. On the other hand, the out-of-pocket expenses for hydroxyurea can be over 35 times higher.
‘Significant challenges’
Experts claim that the exorbitant expense of gene therapies poses an overwhelming barrier due to these harsh realities. The cost of sickle cell treatments in the U.S. is $3.1 million and $2.2 million, respectively, although the prices for gene therapies may differ depending on the country.
Administering the treatments can be just as challenging.
Patients must go to the hospital, where stem cells are removed from their blood in a process that requires specialized equipment. One treatment, made by Vertex Pharmaceuticals and CRISPR Therapeutics, involves sending the cells to a lab as quickly as possible to keep them fresh and using a gene-editing tool called CRISPR to knock out a gene. The cells must be sent back in liquid nitrogen, so they stay frozen until they’re ready to use.
Bluebird Bio manufactures a different therapy that does not utilize CRISPR, but still follows a similar procedure for patients. In both scenarios, patients are required to receive chemotherapy prior to receiving their modified cells through intravenous administration and may need to stay in the hospital for several weeks. The entire process can take several months.
Dr. David Altshuler, the chief scientific officer at Vertex, explained that in numerous regions of the world, the necessary infrastructure is lacking to enable this possibility. He noted that while there is a high demand for it, there are also notable obstacles to overcome.
Many medical facilities not only lack specialized equipment, but also have relatively minimal health care systems. For instance, according to data from the World Health Organization, India and Tanzania have less than a quarter of the hospital beds per capita compared to the United States.
One potential approach, suggested by researchers, is to create more user-friendly alternatives to the newly developed treatments. According to Altshuler, the pharmaceutical company Vertex is actively searching for methods to achieve the same results without the need for chemotherapy, which can have detrimental effects like causing infertility. His team is currently focusing on developing a pill that can stimulate the production of fetal hemoglobin, as opposed to editing genes, as a means to address the defective adult hemoglobin found in individuals with sickle cell disease.
Additional researchers are currently focusing on more straightforward remedies, such as Dr. Stuart Orkin who played a key role in the creation of the Vertex treatment.
Orkin expressed uncertainty about the affordability of future treatments, such as pills.
The Harvard Medical School professor of pediatrics, who receives compensation from the Howard Hughes Medical Institute, which also funds The Associated Press’ Health and Science Department, stated that there will likely be a desire for compensation for the creation of the pill. However, organizations may assist in making it available in developing countries. According to experts, governments will also play a key role in ensuring that treatments reach those in need.
Dongre expressed his desire for gene therapy to be available for sickle cell in India. He would like his children to be among the first to receive it. Mazeze stated that she may wait to see the results of other patients, but she is also considering it for her son.
They both reached a consensus that patients, regardless of their country’s economic status, should have the choice.
According to Dongre, we are all members of a singular planet.
Source: voanews.com